Hives in New York, NY
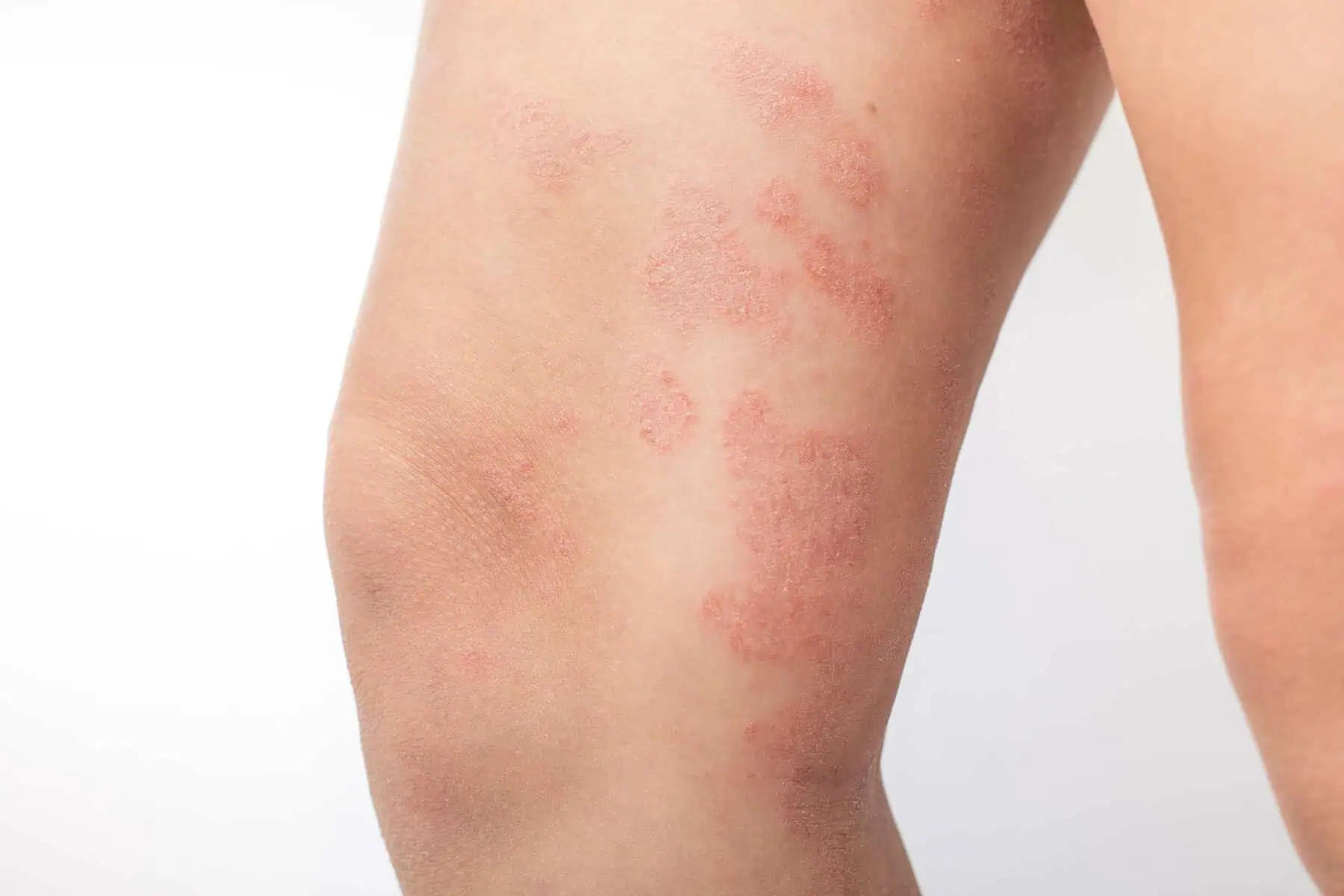
Hives in New York, NY
Hives, also known as urticaria, are a common skin condition characterized by raised, itchy welts that vary in size and appear anywhere on the body. They can be red or skin-colored and often occur suddenly. While they may fade within a few hours, hives can persist for several days or recur frequently, depending on the underlying cause. The condition occurs when the body releases histamines in response to various triggers, leading to blood plasma leaking out of small blood vessels in the skin. Hives can be acute, lasting less than six weeks, chronic, persisting for more than six weeks, or recurring over months or years. While they are typically not life-threatening, severe cases can involve swelling of the throat or face, known as angioedema, and require immediate medical attention.
What Causes Hives?
Hives can be triggered by a wide range of factors, including:
Allergic Reactions
Foods like nuts, shellfish, eggs, and dairy, as well as medications such as antibiotics and nonsteroidal anti-inflammatory drugs (NSAIDs), can trigger allergic reactions leading to hives. Insect stings or bites may also cause hives in sensitive individuals.
Environmental Factors
Temperature extremes, such as heat or cold, sunlight, or physical pressure on the skin, can provoke hives. Exercise and sweat are other potential triggers.
Stress
Emotional stress and anxiety can exacerbate hives or trigger outbreaks in some people.
Infections
Viral infections, such as the common cold or hepatitis, and bacterial infections, including urinary tract infections, can result in hives as the body’s immune system responds.
Idiopathic Causes
Sometimes, the exact cause of hives cannot be determined, leading to a diagnosis of idiopathic urticaria. This form can be particularly challenging to manage without identifying specific triggers.
Identifying and understanding these triggers is crucial for managing and preventing hives, especially in individuals prone to chronic episodes. A detailed medical history and allergy testing can help pinpoint specific allergens or factors contributing to hives outbreaks.
What Are the Different Procedures for Hives?
Managing hives involves a combination of treatments to relieve symptoms and prevent future episodes. Here are some standard procedures and treatments:
Antihistamines
Antihistamines are the first line of treatment for hives. These medications work by blocking the action of histamine, a chemical responsible for allergy symptoms. Over-the-counter antihistamines like cetirizine (Zyrtec), loratadine (Claritin), and diphenhydramine (Benadryl) are commonly used. In cases of chronic hives, healthcare providers may recommend prescription-strength antihistamines or a combination of medications to achieve better control.
Corticosteroids
Oral corticosteroids like prednisone are prescribed for severe or persistent hives to reduce inflammation and suppress the immune response. These medications are effective but are generally used for short periods due to potential side effects, including weight gain, increased blood pressure, and weakened bones with long-term use.
Epinephrine
In situations where hives are part of a severe allergic reaction or anaphylaxis, an epinephrine injection is administered to counteract the reaction quickly. Epinephrine can help reduce swelling, ease breathing difficulties, and prevent potentially life-threatening complications. Individuals at risk for anaphylaxis are often advised to carry an epinephrine auto-injector.
Avoidance of Triggers
Identifying and avoiding known triggers is a crucial strategy for preventing hives. This may involve dietary modifications, avoiding specific medications, or taking precautions to minimize exposure to external factors such as pollen, dust mites, or pet dander.
Cool Compresses and Oatmeal Baths
Applying cool compresses to the affected area or taking oatmeal baths can relieve itching and swelling. These home remedies are safe and can be used alongside medical treatments to enhance comfort.
Modifications
Stress reduction techniques, such as meditation, yoga, or counseling, can help manage hives triggered or worsened by stress. Regular exercise and a balanced diet contribute to overall health and may reduce the frequency of outbreaks.
What Are the Results of Treating Hives?
Treating hives primarily aims to relieve itching and swelling while preventing future outbreaks. With appropriate treatment, most individuals experience significant symptom improvement within a few hours to days. Chronic hives may require ongoing management with antihistamines or other medications to maintain comfort and quality of life.
Successful treatment of hives leads to several positive outcomes, including:
Reduction in Itching and Discomfort
Treatment alleviates the intense itching associated with hives, providing much-needed relief.
Decreased Swelling and Redness
Effective management reduces the swelling and redness of welts, restoring the skin’s appearance.
Prevention of Recurrence
Identifying and avoiding triggers helps prevent future outbreaks, especially in chronic hives.
Improved Quality of Life
Managing hives reduces discomfort and stress, allowing individuals to engage in daily activities without interruption.
Enhanced Sleep Quality
Reducing itchiness improves overall health and well-being.
If you are experiencing hives and seeking relief, consider visiting Park Plaza Dermatology in New York, NY. We offer comprehensive care to ensure your comfort and well-being. Book an appointment today to treat hives!
Benefits of Treating Hives
- Reduces itching
- Decreases swelling
- Prevents recurrence
- Improves quality of life
- Provides emergency relief
- Supports long-term management
- Customizable treatment options
- Promotes better sleep
- Facilitates rapid recovery
- Enhances overall health
Frequently Asked Questions
Hives are raised, itchy welts that appear suddenly and typically resolve within hours to days. Eczema is a chronic skin condition manifested by dry, inflamed, and itchy skin patches. While both conditions involve skin irritation, their causes, symptoms, and treatments differ. Eczema often requires ongoing management with moisturizers and topical medications, whereas hives may resolve more quickly with antihistamines.
Yes, it is possible to have both hives and eczema simultaneously. Hives may appear as a response to specific triggers, while eczema is a chronic condition linked to genetic and environmental factors. Managing both conditions may require a combination of treatments tailored to individual needs.
Showering with cool or lukewarm water can help soothe the itching and lessen the inflammation associated with hives. Hot water should be avoided, as it can exacerbate symptoms. Using gentle, fragrance-free soaps and moisturizers after showering can further alleviate discomfort.
Yes, wool can irritate the skin and trigger hives in individuals with sensitivities. The coarse fibers can cause friction and provoke an allergic reaction, resulting in welts. To prevent irritation, individuals prone to hives may opt for softer fabrics or wear a barrier layer underneath wool clothing.
Both allergists and dermatologists can diagnose and treat hives. An allergist may be more suitable if the hives are suspected to be related to allergies, whereas a dermatologist can address skin-specific concerns. Having a consultation with your healthcare provider can help determine the appropriate specialist based on the nature and triggers of the hives.
Makeup can cause hives if it contains ingredients that trigger an allergic reaction. Fragrances, preservatives, and certain chemicals may irritate the skin and lead to welts. Choosing hypoallergenic or dermatologist-tested products can reduce the risk of a reaction, and performing patch tests before using new products is recommended for those with sensitive skin.
