Psoriasis in New York, NY
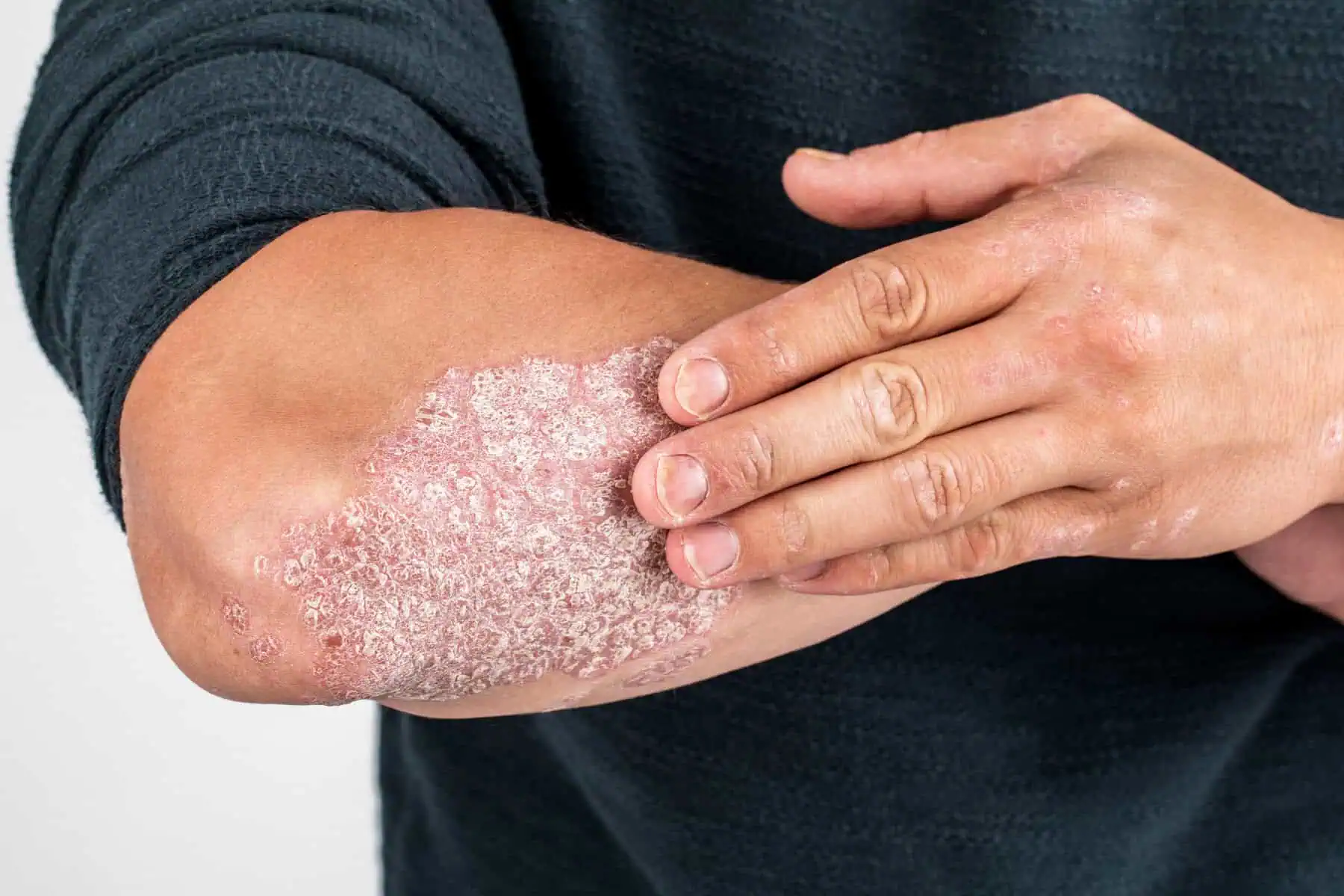
Psoriasis in New York, NY
Psoriasis is a chronic skin condition characterized by red, inflamed patches covered with silvery-white scales. This chronic disorder occurs when the immune system mistakenly accelerates the life cycle of skin cells, resulting in a buildup of rough, scaly plaques that can itch, crack, or become painful. Psoriasis can develop anywhere on the body, including the scalp, elbows, knees, back, or nails, and varies in severity from small, dry spots to widespread inflammation.
At Park Plaza Dermatology in New York, NY, our experienced dermatology providers specialize in diagnosing and managing psoriasis using evidence-based medical treatments and advanced therapies. With multiple locations across Midtown, Uptown Manhattan, West Harlem, Washington Heights, the Bronx, and Brooklyn (Greenpoint), we make it easy for patients to access personalized care that restores comfort and confidence.
What Is Psoriasis?
Psoriasis is an autoimmune skin condition in which the body’s immune system sends faulty signals, causing the skin cells to regenerate too quickly. Instead of renewing over weeks, skin cells rise to the surface within days, forming thickened patches that flake and irritate the surrounding skin. These plaques can appear dry and scaly, often accompanied by redness, itching, and discomfort.
Several forms of psoriasis exist. Plaque psoriasis, the most common type, presents as raised, scaly plaques that can occur on any area of the body. Guttate psoriasis appears as small, drop-like lesions often triggered by infections, while inverse psoriasis develops in skin folds and may cause smooth, shiny patches rather than scaling. More severe forms, such as pustular or erythrodermic psoriasis, can cover large portions of the body and require urgent medical care.
Scalp psoriasis, which often overlaps with these types, is one of the most common manifestations. It produces dense scales along the scalp and hairline, sometimes extending to the forehead, neck, or behind the ears. While it can resemble severe dandruff, scalp psoriasis typically causes more pronounced redness and discomfort.
Common Areas of Psoriasis
Psoriasis can appear in various areas of the body and present in different forms. The most commonly affected regions are visible and often cause both physical discomfort and emotional distress.
Scalp
Characterized by flaking, scaling, and redness along the hairline.
Elbows and Knees
Typically develop thick, scaly plaques that can itch or crack.
Nails
May show pitting, discoloration, or brittleness.
Torso and Back
Widespread patches that can vary in size and severity.
Hands, Feet, and Groin
Sensitive areas prone to irritation and pain.
Causes and Triggers
Psoriasis results from an overactive immune response that is influenced by both genetic and environmental factors. Identifying triggers is crucial for preventing flare-ups and maintaining clear, healthy skin.
- Stress and anxiety
- Skin injuries such as cuts or burns
- Infections (especially strep throat)
- Certain medications (like beta-blockers or lithium)
- Cold, dry weather
- Hormonal changes and alcohol use
Symptoms and Diagnosis
Psoriasis is typically diagnosed based on its distinct appearance and patient history. Symptoms may include thick, raised plaques covered with silvery-white scales, redness, flaking, itching, or even pain. Some patients may notice small cracks or bleeding where plaques are most inflamed.
During your visit, one of our experienced dermatology providers will conduct a thorough skin evaluation and discuss your symptoms and medical history. In some cases, a skin biopsy may be performed to confirm the diagnosis and rule out similar conditions such as eczema or fungal infections. Understanding the specific type and severity of psoriasis helps us design a treatment plan that targets both your symptoms and their underlying causes.
Treatment Options
At Park Plaza Dermatology, we offer a range of safe and effective treatments tailored to each patient’s skin type, condition, and lifestyle.
Topical Therapies
Corticosteroids, vitamin D creams, and medicated shampoos reduce inflammation and scaling.
Phototherapy
Controlled exposure to UV light slows the rapid growth of skin cells.
Systemic Medications
Oral or injectable options, such as methotrexate or biologic therapies, are available for moderate-to-severe psoriasis.
Lifestyle and Supportive Care
Moisturizers, stress management, and trigger control help maintain long-term results.
What to Expect
The psoriasis treatment process begins with a consultation and thorough skin evaluation. During this visit, our dermatology providers will review your medical history, discuss potential triggers, and recommend the most suitable treatment for you.
Once treatment begins, improvement is typically gradual. Topical and light-based therapies can take several weeks to show visible results. Biologic treatments may take several months to reach their full effect. Many patients see reduced redness and scaling within four to six weeks of consistent care. Over time, plaques soften, itching lessens, and the skin becomes smoother and healthier.
Regular follow-up visits are important to monitor progress and make any necessary adjustments. Because psoriasis is a chronic condition, maintenance treatment is often recommended even when symptoms have cleared to prevent relapses.
Benefits of Treatment
Effective psoriasis management can dramatically improve both physical comfort and emotional well-being. By reducing inflammation, scaling, and itching, treatment helps restore the skin’s natural texture and appearance while decreasing the frequency and intensity of flare-ups. Beyond the cosmetic improvements, proper management also protects against secondary complications such as infections and psoriatic arthritis.
Our goal at Park Plaza Dermatology is long-term control, not just temporary relief. We empower patients through education, personalized plans, and ongoing support. Our focus is on helping to maintain clear, healthy skin and improve overall quality of life.
Safety, Risks, and Side Effects
All psoriasis treatments are carefully prescribed and monitored to ensure safety. Topical medications are generally well-tolerated, although overuse of corticosteroids can cause skin thinning or discoloration. Phototherapy may result in mild redness or dryness, whereas systemic medications require regular laboratory tests to monitor liver, kidney, and immune function.
Our providers always aim to minimize side effects. We customize dosages and adjust regimens as needed. Patients also receive education on proper application and sun protection. Excessive sun exposure or improper product use can exacerbate psoriasis.
Frequently Asked Questions
No, psoriasis is not contagious. It is an autoimmune condition and cannot be transmitted through physical contact.
While there is no definitive cure, many patients achieve long-term remission with modern treatments, lifestyle adjustments, and maintenance care.
Yes, scalp psoriasis often responds best to medicated shampoos and topical solutions designed specifically for the scalp’s unique environment.
Yes. Stress is one of the most common triggers for flare-ups. Incorporating stress management techniques can significantly improve treatment outcomes.
Why Choose Park Plaza Dermatology for Psoriasis Care
Park Plaza Dermatology is a trusted place for comprehensive psoriasis care in New York City. Our experienced dermatology providers specialize in both medical and cosmetic dermatology. We offer patients the most advanced treatments available. Each care plan is tailored to the individual. We combine the latest therapies with an understanding of each patient’s skin history, lifestyle, and goals.
We proudly serve patients throughout Midtown, Uptown Manhattan, West Harlem, Washington Heights, the Bronx, and Brooklyn (Greenpoint). Our facilities provide accessible and compassionate care in modern settings. With a patient-centered approach and focus on long-term results, Park Plaza Dermatology helps people regain control over their skin and confidence in their appearance.
Schedule Your Psoriasis Consultation Today
Take the first step toward clear, healthy skin with expert psoriasis treatment at Park Plaza Dermatology in New York, NY. Whether you’re managing mild flare-ups or severe symptoms, our team can help you find relief with personalized care and the latest advancements. Schedule your appointment or verify your insurance today. Begin your journey toward better skin health and an enhanced quality of life.
